The global healthcare system is full of problems and inefficiencies, and at the forefront of those issues lies the question: “where do we even begin?” Eliminating waste has become a common refrain, but which sources of waste should be dealt with first? Nowhere are these problems more evident than in the United States, a country is burdened by increasingly complex systems for payments and claims verification, as well as much heavier regulations than other comparable countries.
In the U.S. alone, Billing and Insurance-Related (BIR) costs total up to $496 billion a year and represent 15% of total healthcare spending, with as much as half of the cost being unnecessary, according to the National Academy of Medicine (NAM). The majority of this cost goes to administrative expenses and salaries, with the average healthcare organization in the U.S. requiring 770 full-time administrative workers per $1 billion in revenue collected—a ratio that is over seven times higher than that of other industries.
|
$496 B The annual cost of healthcare billing and insurance-related processes in the U.S. |
15%
Of BIR costs considered to be unnecessary under more efficient models |
7.7x More administrative workers required in healthcare than in other industries, due largely to claims verification nightmares |
Yet, much of this enormous cost is frivolous. The National Academy of Medicine estimates that as much as half of BIR costs would be unnecessary under a more efficient system, while the Harvard Business Review estimates that reducing administrative complexity, fraud, and excessive prices charged by inefficient healthcare providers would save the U.S. healthcare system over $500 billion.
While there is plenty of bureaucracy, regulation, and payment processing headaches to blame, the healthcare system is essentially suffering from a giant identity crisis. Fraud and excessive prices stem from administrative complexity across the claims verification process, which exists due to the number of parties involved in providing and paying for healthcare and the difficulty those parties have in identifying and checking each other’s work.
Imagine a giant game of “telephone” between healthcare providers, insurance agencies, clearinghouses, and payment processors, and you’ve got an idea of what settling a payment claim involves.

The healthcare system is essentially suffering from a giant identity crisis
Empowering all of these parties with digital ID would be like adding caller ID and voicemail to that game of telephone—everyone would have a much easier time conveying messages and understanding what’s going on. A report on digital identification from the McKinsey Global Institute points to the potential for up to 90% reduction in onboarding costs and $1.6 trillion in global savings from payroll fraud through the adoption of strong models for digital identity.
To better understand how digital identity can help remove friction from the processing of payment claims in healthcare, this article explores how the medical claims verification process works, where the major sources of waste arise, and what new technologies for digital identity can offer to help solve these problems.
How the claims verification process works
When a patient sees a healthcare provider, the services they receive get recorded using special codes developed to standardize communications in the medical field. The International Classification of Disease (ICD) covers the diagnosis of illnesses, including symptoms and causes of death, while Current Procedural Terminology (CPT) identifies the services provided to a patient so insurance companies can evaluate a claim. Medical coders use these codes to describe what services the patient received. A medical billing specialist then combines that data with information about the patient and their insurance provider to create a payment claim that can be sent off to the insurance agency.
Still with us? It gets even more complicated…
The software used to create an insurance claim must conform to standards mandated by HIPAA. Most payment claims are digital, but paper claims have not yet been eliminated so medical coders and billing specialists need to be able to file both types of claims. Some healthcare providers use software that helps ensure the legibility and accuracy of documents and standardized forms to speed the process, but entering information correctly is only the first potential source of errors in the claims process.
Once a claim has been prepared, it doesn’t actually go straight to the insurance agency. A healthcare provider will typically send the claim to a clearinghouse that double-checks the information and then routes the claim to the appropriate insurance agency. Insurance providers each have their own standards for submitting claims, so sending their payment claims to a clearinghouse helps healthcare providers ensure that their claims meet each insurance agency’s specific requirements.
From there, the payment claim bounces between a series of insurance companies and third-party payment processors. Once the claim has been evaluated, the insurance agency provides the patient and healthcare provider with an Explanation of Benefits (EOB). The EOB includes the agency’s evaluation of the information shared by the healthcare provider about what services the patient received, how much the agency will pay the healthcare provider, and how much the patient owes their provider.

Not including the patient and her family, that’s a minimum of four parties each claim goes through.
And of course, multiply that whole process by the number of doctors your hospital employs and the 19 patients per day the average doctor sees, and it’s not difficult to see why healthcare is so admin-heavy.
Identifying sources of waste
The bulk of the half-trillion in annual BIR costs fall on healthcare providers, who take on about twice as much as insurance agencies. Behind both providers and insurers are the public programs, which still pay over $50 billion a year in BIR costs in the U.S. alone.
A number of factors contribute to excessive costs, but the underlying theme of these problems lies in data reconciliation. The number of parties involved in creating and processing a payment claim, as well as the volume of claims generated on any given day, creates an administrative nightmare. Processing claims involves recording and verifying lots of redundant information, which inevitably results in lots of errors. Dealing with those errors takes extra time, an expense that gets passed on to all parties down the line.
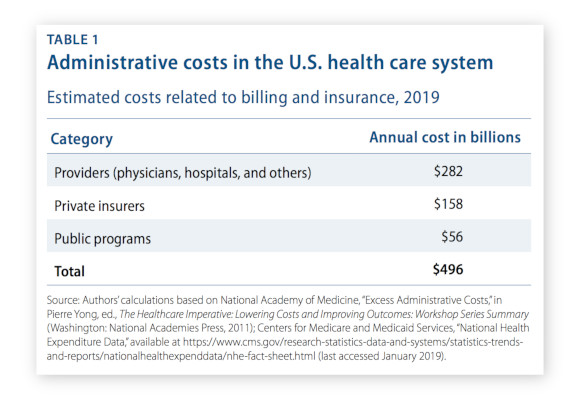
Source: Center for American Progress, 2019
Factors that contribute to BIR costs include:
Complexity
In The Healthcare Imperative: Lowering Costs and Improving Outcome, author James G. Kahn outlines the work that healthcare providers have to deal with to process an insurance claim:
“contracting with insurers and subcontracted providers; maintaining benefits databases; determining patient insurance and cost sharing; collecting copayments, formulary, and prior authorization; coding of services delivered; checking and submitting claims; receiving and depositing payments; appealing denials and underpayments; collecting from patients; negotiating end-of-year resolution of unsettled claims; and paying subcontracted providers.”
I don’t know about you, but I’m exhausted after just reading that list.
Each of these steps requires multiple parties to communicate and verify sensitive information. A single mistake at any point in the process has cascading effects on the rest of the parties that come in contact with a claim. Once an error has been discovered, it needs to be traced to its source so the correct information can be identified and the claim can continue being processed.
Variation
It’s important to distinguish the complexity involved with the claims verification process in general from the complexity introduced by the variation between plans and benefits offered by insurance companies. In addition to their standard product offerings, insurance agencies often customize plans for larger organizations. Healthcare providers have to keep track of which plan each patient has, as well as what benefits each plan offers. Patients need to be able to rely on healthcare providers to provide accurate estimates of their healthcare costs, but the complexity involved often leads to mistakes.
And when patients can’t cover their bills, the burden falls on everyone else—providers, insurance agencies, and taxpayers.
Friction
Many of the steps involved in processing payment claims come with their own unique quirks that can delay or create problems in the settlement of a claim. Priority authorization and high rates of initial non-payment and underpayment all contribute to delays in final payment. Dealing with errors that come up during the processing of claims requires its own workflow that introduces extra complexity to the settlement of claims.
Fraud
Fraud occurs when the individuals involved in creating and processing a claim take advantage of the lack of oversight in the system to charge money for unnecessary or non-existent services. Title II of HIPAA, referred to as the “Administrative Simplification” section, outlines the actions healthcare providers and insurance agencies have to take in order to ensure data privacy for patients and avoid fraud. Unfortunately, the regulations fail to address a number of loopholes exploited by corrupt providers and insurance companies.
Among healthcare providers, fraud typically occurs when providers bill insurance agencies for services they never provided or mark-up their payment claims with more expensive services. Some of the worst offenders actually recommend and perform unnecessary services on patients. On the other end, insurance companies have been accused of purposefully complicating claims processing to promote higher levels of non-payment and underpayment.
Waste
The problems that healthcare providers and insurance agencies introduce into the claims verification process aren’t always intentional; even professionals make mistakes. The number of hands a claim must pass through and the number of actions that must be taken in the course of settling a payment claim introduces multiple opportunities for error. Unnecessary medical services, improper usage of medical devices, and errors in data entry and verification all contribute to waste in the healthcare system. The gap between best practices and the care delivered takes time to close, but the lack of standardization leads healthcare providers to deliver ineffective services until their processes can be updated.
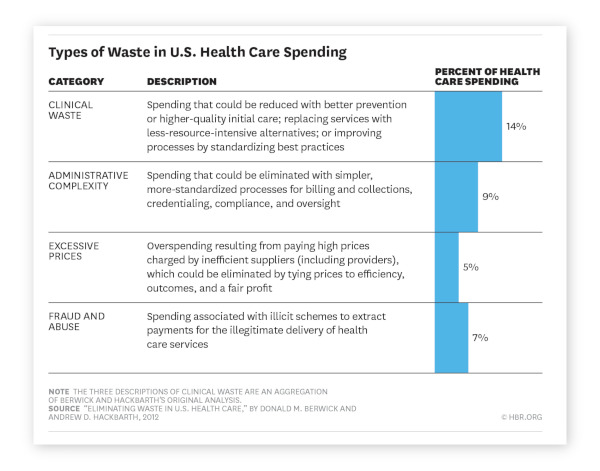
Source: HBR, 2015
How can digital identity help with claims verification?
Tools for digital identity are currently in the midst of an evolution. A new model for digital identity called “decentralized” or self-sovereign” identity holds the potential to transform the way people interact with each other in the digital world. The Internet made it possible to share information across the globe at the click of a button, but (initially) lacked a standardized layer for identity. As a result, it remains difficult to tell where information comes from. Providing the parties involved in processing insurance claims with tools for decentralized identity can make it easier for everyone to communicate and understand where a claim has been and what needs to be done to finish processing it.
To better understand decentralized identity, it helps to have a sense of how previous models for digital identity have developed over the years. Here’s a brief explanation of the different stages in the development of digital identity technology:
1. Siloed Identity
In the beginning, there were usernames and passwords. When websites needed to separate private information from public information and most people only visited a handful of websites, this simple system provided an easy fix. We refer to it as “siloed” because every website and all of its users have to maintain their own data silos to remember all of their usernames and passwords.
2. Federated Identity
As people came to use more websites and mobile applications, they began to need spreadsheets and password managers to help keep track of all of their usernames and passwords. Single Sign-On (SSO), an early form of federated identity, was developed to allow people to use the same set of credentials for different services in the same online ecosystem. For example, being able to use your Gmail account to access Youtube and Google’s other products counts as a form of SSO. In this case, Google serves as your Identity Provider (IDP), trusted by websites that opt-in to this SSO system.
Federated identity takes SSO a step further by allowing people to use the same login information across different services in different ecosystems. When you see a button that says “Sign in with Google” or “Sign in with Facebook,” you’re seeing an example of federated identity.

3. Decentralized Identity
Decentralized identity rejects usernames and passwords as the basis for digital identity and works to enable us to carry and use credentials on our mobile devices as easily as we use the licenses, credit cards, and other forms of ID we keep in our wallets.
At the heart of decentralized identity lies digital wallets, like Connect.Me. Digital wallets developed using protocols for decentralized identity enable people to make verifiable claims about themselves using credentials that can be stored, shared, and backed-up using their digital wallet application.
In the same way someone can use a barcode on the back of a driver’s license to tell if it’s fake or not, credentials made using protocols for decentralized identity come with a reference recorded on a distributed ledger containing the information necessary for someone to verify the authenticity of a claim.
Contrary to popular belief, decentralized or self-sovereign identity does not involve putting sensitive information on a distributed ledger (such as a blockchain) or allow people to “self-attest” to facts about themselves.
Those developing the standards for decentralized identity aim to add that missing identity layer to the internet. Going back to the theme of data reconciliation, communication and verification represent the two weak points involved in settling payment claims. Any time a provider, insurance agency, clearinghouse, or payment processor does anything involving a payment claim, the actions must be recorded so that errors can be traced back to their source. Instead of relying on all of the parties involved in processing a payment claim to be trustworthy, providing them with tools for decentralized identity makes it easier to tell who did what and perform audits as necessary.
Adopting tools for decentralized identity can help the entities involved in processing payment claims identify and enable secure communication between the organizations and staff involved in processing a particular payment claim. Allowing customers to manage their own identity allows these organizations to refer to a single source of truth with regard to patient data rather than each organization relying on its own data silo. Reducing the friction involved in communicating the information needed to process payment claims helps decrease the costs associated with processing claims.
The Institute of Medicine estimates that healthcare providers lose $20-$30 billion a year to errors that arise in the claims verification process. We’re not just talking about financial losses either; those errors also result in an estimated 400,000 preventable deaths a year, with almost 100,000 from the U.S. alone. Adopting new technologies that make it easier to record and verify the information needed to process payment claims can help save money and lives.
Less time on admin, more on patient care
When discussing the elimination of wasteful spending in healthcare, it’s critical to ensure that we’re doing so in ways that don’t decrease the quality of care for patients. It’s important to note that the point of eliminating waste in healthcare spending isn’t to achieve the lowest possible level of administrative spending. Researchers Robert A. Berenson and Bryan E. Dowd point out that administrative spending in Medicare may actually be too low—their work suggests that greater investment in the administration of healthcare would actually improve efficiency.
In his report on excessive healthcare costs, Kahn notes that reducing BIR costs requires a two-sided approach. Some healthcare providers do a far better job of managing BIR expenditures than others, so while most of the potential savings on BIR costs can be achieved by simplifying the claims process, some healthcare providers may see even greater savings by simply adopting the best practices of more efficient providers. Developing a straightforward claims verification process is only half the battle; empowering the individuals involved in claims processing with the best technologies available represents the other half.
Adopting tools for decentralized identity will help eliminate wasteful spending and allow healthcare providers to spend less time on administrative work and more time on patient care. In order to make sense of healthcare, we need to provide a way to identify—and verify—the people and organizations responsible for delivering it.

Getting started with decentralized identity
Ready to take the next step and start slashing BIR costs and freeing up staff time for what matters most?
At Evernym, we can help put your organization on a fast-track to decentralized identity through our Early Access Program. Our team (the same team that co-invented the Decentralized Identifier (DID) standards and designed Hyperledger Indy and Sovrin) will work with you to evaluate, build, and test a use case unique to your organization. You’ll cut months out of your learning and have the opportunity to collaborate with a cross-sector community of nonprofits, businesses, and governments pioneering the future of digital identity.
To see if the Early Access Program is right for you, fill out the form below and we’ll schedule a quick call to go over the program and how decentralized identity fits within your greater business strategy:
Request information on our Early Access Plan“This program has put Truu at the forefront of decentralized healthcare identity. We have worked closely with Evernym to enable doctors to control their own portable digital identities at a higher level of trust than current standards.” – Dr. Manreet Nijjar, Co-Founder, Truu
|